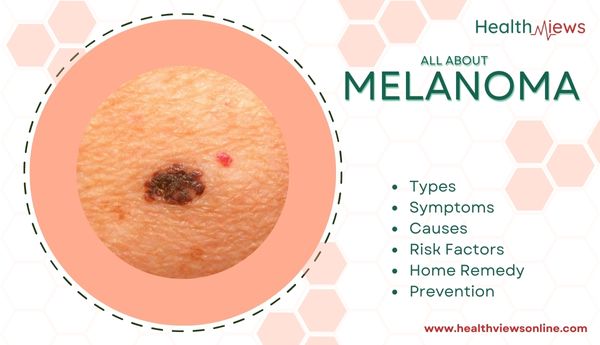
What is Melanoma?
Melanoma, which means “black tumor,” is the deadliest form of skin cancer. It multiplies rapidly and has the ability to spread to any organ.
Melanoma, a type of skin cancer, is often referred to as the “most serious skin cancer” because it can spread from the skin to other parts of the body.
Skin cells called melanocytes are what cause melanoma. These cells are responsible for the production of melanin, the dark pigment that gives skin its color. The majority of melanomas are black or brown, but some are pink, red, purple, or skin-colored.
Also Read: All About Rosacea: Types, Symptoms, Causes, Prevention, Home Remedies
Types
Melanoma skin cancer comes in 4 primary types:
- Superficial spreading melanoma: This is the most common type of melanoma, and it frequently affects the trunk or limbs. Cells grow slowly at first before spreading across the skin’s surface. Source
- Nodular melanoma: This second most prevalent kind of melanoma can develop on the neck, head, or trunk. It might be reddish or blue-black in color and grows more quickly than other varieties. Source
- Lentigo malignant melanoma is less frequent and more likely to appear in older adults, especially on areas of the body like the face that have been exposed to too much sun over an extended period. As people age, their chance of developing this type of melanoma may rise due to repeated sun exposure. Source
- Acral lentiginous melanoma: Acral lentiginous melanoma is rare cancer that can affect people of all races and ethnicities. It is the most common type of melanoma in African and Asian people. It can appear on the palms of the hands, the soles of the feet, and even under the toenails and fingernails. Source
Causes
Melanoma develops when UV-induced DNA damage from sunburns or tanning causes changes (mutations) in melanocytes, resulting in uncontrolled cellular growth.
Sunlight is the primary source of UV rays, however artificial sources like tanning beds can also emit some of them. While some DNA damage from UV radiation may occur in the few years before the development of cancer, a large portion of it may result from exposures that occurred many years earlier.
Risk factors
Scientists are aware that some skin types are more prone to melanoma than others.
The following elements could also raise the risk of skin cancer:
- A high density of freckles or a propensity to develop freckles after sun exposure to a large number of moles
- Five or more unusual moles
- Actinic lentigines, also known as liver spots or age spots, are present.
- Giant congenital melanocytic nevi are brown birthmarks
- Pale skin that does not tan easily and burns easily.
- High sun exposure, particularly if it causes blistering sunburn, and if sun exposure is intermittent rather than regular older age
- Older age
- Light eyes
Symptoms
Melanoma is a type of skin cancer that can manifest itself in a variety of ways on the skin. It can resemble:
- Changing the mole
- The spot that appears to be a new mole, freckle, or age spot but differs from the others on your skin
- Spot with a jagged border, and multiple colors, and that is growing
- Dome-shaped growth that feels firm and may resemble a sore that bleeds
- Vertical dark brown or black line beneath a fingernail or toenail
- A darker band of skin around a fingernail or toe
- A scar-like patch of thick skin that is slowly growing
Dermatologists developed the ABCDEs of melanoma to assist people in detecting a possible melanoma on their skin:
- Asymmetry – The spot’s two halves are not identical.
- Border – The border of the spot is irregular, scalloped, or poorly defined.
- Color – The color of the spot varies from one area to the next, with shades of tan, brown, or black, as well as areas of white, red, or blue.
- Diameter – While melanomas are typically larger than 6 millimeters, or about the size of a pencil eraser, they can be smaller when diagnosed.
- Evolving – The spot appears to be different from the others or changes in size, shape, or color. Source
Diagnosis
Dermatologists can assist people in identifying a potential melanoma on their skin. Inspecting your skin will typically be the first step in melanoma diagnosis.
Some general practitioners photograph a suspected tumor digitally to submit the images to a specialist for review.
Many general practitioners only encounter melanoma cases every few years due to the disease’s relative rarity. It’s important to keep an eye on your moles and visit your doctor if anything changes. It will be easier to diagnose if you take pictures to document any changes.
Treatment
Your doctor can stage your melanoma using a number of tests. Your physician might carry out the following tests:
- Biopsy of a sentinel lymph node:
- CT scan for computed tomography
- Scan using magnetic resonance imaging (MRI)
- Scan using a positron emission tomography (PET)
- Blood test
The other melanoma treatment options include:
- Lymphadenectomy
- Immunotherapy
- Targeted therapy
- Chemotherapy
- Radiation therapy
- Clinical trial
- Adoptive T-cell therapy
- Palliative care
When to see a doctor
If melanoma is detected, you will be directed to a dermatology clinic for additional testing. After visiting your general practitioner, you should make an appointment with a specialist within two weeks.
The mole and the rest of your skin will be examined by a dermatologist or plastic surgeon. To find out if the mole is cancerous, it may be excised and submitted for a biopsy. A local anesthetic is typically used during a biopsy to numb the region surrounding the mole so you won’t feel any pain.
Also Read: Basal cell carcinoma: Types, Causes, Risk Factors, and Treatment
Prevention
- The best time to avoid the sun and seek shelter is between 10 and 4 o’clock.
- By avoiding excessive sun exposure and sunburns, you may lower your risk of developing melanoma.
- Avoid tanning beds. Instead, use a cosmetic spray tan.
- Wear wide-brimmed hats, sunglasses, long-sleeved shirts, and clothing whenever you can.
- Use a broad-spectrum sunscreen with an SPF of 30 or higher, and reapply frequently, typically every 1.5 hours or more frequently if you’re exercising or perspiring.
- Use a lip balm that contains sunscreen.
- For infants older than six months and small children, don’t forget to use sunscreen. Source
Want to know about other skin disorders? Check out Skin Problems on Health Views Online.