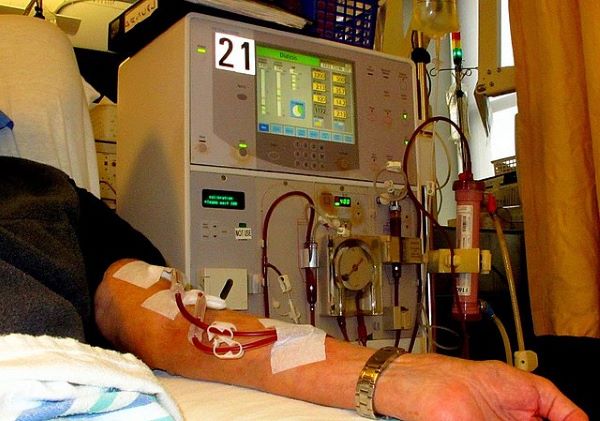
What is Dialysis? Dialysis is a medical procedure that helps perform some of the functions of healthy kidneys when they are unable to do so. It is a treatment option for individuals with kidney failure or end-stage renal disease (ESRD), a condition where the kidneys are no longer able to effectively filter waste products and excess fluids from the blood.
Also Read: What Is Chronic Kidney Disease? Causes, Symptoms & Treatment
There Are Two Primary Types of Dialysis:
Hemodialysis: This is the most common form of dialysis. During hemodialysis, the patient’s blood is circulated outside their body through a machine called a dialyzer or artificial kidney. The dialyzer acts as a filter, removing waste products, excess fluids, and toxins from the blood. The cleaned blood is then returned to the patient’s body. Hemodialysis treatments typically take place at a specialized center or hospital three times a week and last for several hours each session.
Peritoneal Dialysis: Peritoneal dialysis is a home-based treatment option that uses the lining of the abdomen, called the peritoneum, as a natural filter. A catheter is surgically placed in the abdomen, and a sterile dialysis solution is introduced through the catheter into the peritoneal cavity. Waste products and excess fluids from the blood pass through the peritoneum into the solution. After a period of time, the solution is drained, taking the waste products with it. Fresh dialysis solution is then added, and the process is repeated several times throughout the day or night.
What are the Benefits of Dialysis? How Does Dialysis Help a Patient With Kidney Failure?
Here are some key benefits of dialysis:
- Removal of Waste Products: Dialysis helps remove waste products, toxins, and excess fluids from the body that the kidneys are unable to eliminate. This cleansing process restores the body’s electrolyte balance and prevents the buildup of harmful substances that can lead to various complications.
- Maintenance of Fluid Balance: Dialysis assists in regulating fluid levels in the body. By removing excess fluids, it prevents fluid overload, which can cause symptoms such as swelling, shortness of breath, and high blood pressure. Maintaining fluid balance helps reduce strain on the heart and improves overall cardiovascular health.
- Management of Electrolyte Levels: Dialysis plays a crucial role in managing electrolyte levels in the body. By removing excess electrolytes and maintaining the proper balance of sodium, potassium, calcium, and phosphate, it helps prevent imbalances that can lead to complications such as irregular heart rhythms, muscle weakness, and bone problems.
- Improved Energy and Well-being: Dialysis helps alleviate symptoms associated with kidney failure, such as fatigue, weakness, and overall malaise. By efficiently removing waste products and toxins, dialysis boosts energy levels and enhances overall well-being, allowing individuals to engage in daily activities and lead a more active lifestyle.
- Reduction of Symptoms: Dialysis can help relieve symptoms commonly experienced by individuals with kidney failure, including nausea, vomiting, itching, and poor appetite. By eliminating waste products and toxins that contribute to these symptoms, dialysis improves the quality of life and provides relief from discomfort.
- Preservation of Kidney Function: Dialysis can help prolong the functioning of the kidneys, even if they are severely damaged. By providing artificial filtration, it allows the kidneys to rest and prevents further deterioration. This can be particularly beneficial for individuals awaiting a kidney transplant or those who are not eligible for transplantation.
- Flexibility and Independence: For individuals undergoing peritoneal dialysis, which can be performed at home, there is increased flexibility and independence. This form of dialysis allows patients to manage their treatments independently, reducing the need for frequent hospital visits and offering greater control over their daily schedules.
- Supportive Care: Dialysis treatments are typically conducted in specialized centers where patients receive care from a dedicated healthcare team. This team, which includes nephrologists, nurses, and dietitians, provides ongoing support, monitoring, and education, helping patients manage their condition effectively and adapt to lifestyle changes.
While dialysis provides significant benefits, it is important to note that it is not a cure for kidney failure. However, it serves as a life-sustaining treatment option that allows individuals to manage their condition, maintain their health, and improve their quality of life while awaiting a kidney transplant or if transplantation is not possible.
What is the General Dietary Guideline for a Patient Undergoing Dialysis?
We can provide a general overview of a diet plan for individuals on dialysis. However, it’s important to note that dietary recommendations may vary based on an individual’s specific needs and health condition. Consulting with a registered dietitian who specializes in renal nutrition is highly recommended for personalized dietary advice. Here are some general principles for a dialysis diet:
- Control Fluid Intake:
- Follow your healthcare team’s recommendations regarding fluid restrictions.
- Monitor your fluid intake carefully, including all beverages and foods with high water content.
- Limit or avoid consuming excessive amounts of liquid-rich foods such as soups, ice cream, gelatin, and juicy fruits.
- Limit Sodium (Salt) Intake:
- Minimize the use of table salt and avoid high-sodium processed and packaged foods.
- Opt for fresh, homemade meals and flavor your food with herbs, spices, and low-sodium seasoning alternatives.
- Be mindful of hidden sources of sodium, such as condiments, canned foods, and pre-packaged snacks.
- Monitor Potassium Intake:
- Limit high-potassium foods, such as bananas, oranges, tomatoes, potatoes, spinach, and avocados.
- Choose lower-potassium alternatives like apples, berries, cabbage, green beans, and rice.
- Soaking certain high-potassium foods (e.g., potatoes) in water before cooking can help reduce potassium levels.
- Manage Phosphorus Intake:
- Restrict foods high in phosphorus, including dairy products, nuts, seeds, chocolate, and carbonated drinks.
- Choose lower-phosphorus alternatives like rice milk, almond milk (watch for phosphorus additives), and white bread.
- Take prescribed phosphate binders with meals as recommended by your healthcare provider.
- Monitor Protein Intake:
- Consume an appropriate amount of high-quality protein to meet your individual needs. The recommendation may vary based on your condition.
- Include lean sources of protein such as skinless poultry, fish, eggs, and low-fat dairy products.
- Limit high-protein foods that are also high in phosphorus, such as red meat and organ meats.
- Consider Energy Intake:
- Ensure you consume enough calories to meet your energy needs. Your dietitian can provide guidance based on your specific requirements.
- Include healthy sources of carbohydrates like whole grains, fruits, and vegetables to provide energy.
- Vitamin and Mineral Supplementation:
- Depending on your lab results, your healthcare team may recommend specific vitamin and mineral supplements like Vitamin D, iron, and vitamin B complex.
Remember, this is a general overview, and individual needs may vary. It’s crucial to work closely with a registered dietitian who specializes in renal nutrition to develop a personalized diet plan tailored to your specific needs and health condition. They will consider factors such as your lab results, dialysis type, and other medical considerations to create an optimal dietary approach for you.
Also Read: All about Iron: Functions, Daily Dose, Deficiency, Sources & Toxicity
Dialysis Can Have Side-Effects too – What are the Side-Effects of Dialysis?
While dialysis is a life-saving treatment for individuals with kidney failure or end-stage renal disease (ESRD), it may also have some side effects. These side effects can vary from person to person and depend on various factors such as the type of dialysis, individual health condition, and the overall management of the treatment. Here are some potential side effects of dialysis:
Low Blood Pressure (Hypotension): During dialysis, fluid removal can cause a drop in blood pressure, leading to symptoms such as dizziness, lightheadedness, nausea, or even fainting. Healthcare providers closely monitor blood pressure levels during dialysis and take measures to prevent or manage low blood pressure, such as adjusting fluid removal rates or medications.
Muscle Cramps: Some individuals may experience muscle cramps, particularly in the legs, during or after dialysis. This can be due to fluid and electrolyte imbalances. Proper hydration, adjusting the dialysis prescription, and medications can help alleviate muscle cramps.
Itching (Pruritus): Dialysis patients may experience skin itching, which can be caused by the accumulation of waste products in the bloodstream. Maintaining good skin hygiene, using moisturizers, and discussing potential treatments with the healthcare team can help manage this symptom.
Infection: Infections can occur at the site where the dialysis access is inserted, such as an arteriovenous fistula or catheter. Additionally, peritonitis (inflammation of the peritoneum) can occur in individuals undergoing peritoneal dialysis. Following proper hygiene practices, keeping the access site clean, and promptly reporting any signs of infection to the healthcare team are crucial for infection prevention and management.
Anemia: Dialysis can sometimes contribute to a decrease in red blood cell production, leading to anemia. This can result in symptoms such as fatigue, weakness, and shortness of breath. Medications, iron supplements, and erythropoiesis-stimulating agents may be prescribed to manage anemia.
Changes in Appetite and Taste: Some individuals undergoing dialysis may experience changes in appetite, taste, or a metallic taste in the mouth. This can affect nutritional intake. Working with a registered dietitian and discussing these changes with the healthcare team can help address these concerns and develop strategies to maintain adequate nutrition.
Emotional and Psychological Effects: Living with a chronic condition and undergoing regular dialysis treatments can have emotional and psychological impacts. Feelings of anxiety, depression, or adjustment difficulties are not uncommon. Support from healthcare professionals, counselors, and support groups can be valuable in managing these aspects of dialysis.
It’s important to note that not all individuals will experience these side effects, and the severity may vary. Healthcare providers closely monitor patients during dialysis sessions, address any concerns or symptoms promptly, and make adjustments to the treatment plan as necessary to minimize side effects and optimize the overall dialysis experience.
If you are undergoing dialysis and experiencing any side effects, it is crucial to communicate with your healthcare team. They can provide appropriate guidance, support, and interventions to help manage these side effects and improve your overall well-being during the treatment.
Conclusion
While dialysis can significantly improve the quality of life for individuals with kidney failure, it is a demanding treatment that requires adherence to a strict schedule and regular medical monitoring. Each type of dialysis has its own advantages, and the choice of dialysis modality depends on factors such as the patient’s health condition, lifestyle, and preferences.
It’s important for individuals considering or undergoing dialysis to consult with healthcare professionals specializing in kidney care for personalized guidance, support, and monitoring throughout the treatment process.
Also Read: What is Arjuna? Uses and Health Benefits of Arjuna
Featured Image Source: Anna Frodesiak, CC0, via Wikimedia Commons