Eczema is a noncontagious inflammatory skin condition that causes dry, red, bumpy, and itchy patches of skin that irritate. These symptoms could be painful, and they may also result in skin color changes and blisters. Your eczema symptoms could become more severe if you come into contact with an allergy or irritant.
What is Eczema?
Eczema is a reaction pattern that the skin produces in a variety of diseases, rather than a specific health condition. It starts with red, raised tiny blisters containing clear fluid on top of red, elevated plaques. When the blisters explode, the affected skin weeps and leeches.
It usually begins in infancy or early childhood and can last into old age. On the other hand, anyone of any age can experience eczema. Some people will have symptoms on and off for the rest of their lives.
Also, Read Skin Disorder: Types Of Skin Disorders You Must Know – Part 1
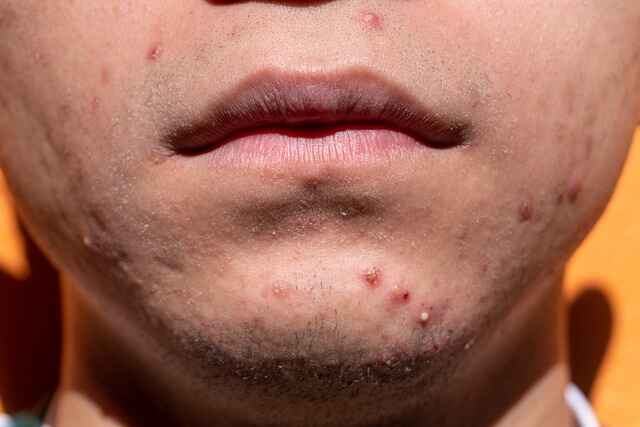
Types of Eczema
Eczema comes in various forms, including the following:
1. Atopic dermatitis
Atopic dermatitis is the kind of eczema that is most prevalent. It usually begins in childhood and gradually fades or disappears by adulthood. Symptoms typically appear in childhood and can range from mild to severe. If one of the kid’s parents has atopic dermatitis, the child is more likely to develop it as well. Atopic dermatitis causes dry skin patches that can become itchy, red, and inflamed. These patches are commonly found in the creases of the elbows and knees, as well as on the face, neck, and wrists.
2. Contact dermatitis
If you have thick, scaly, and reddish skin that is brought on by an allergic reaction to something you touch, you may have contact dermatitis.
There are two kinds of it:
- Allergic contact dermatitis – It is a reaction of the immune system to an irritant, such as latex or metal.
- Irritant contact dermatitis – It develops when a chemical or other substance irritates your skin.
When certain substances come into contact with some people, they develop a skin reaction. Contact dermatitis is more common in people who have atopic dermatitis.
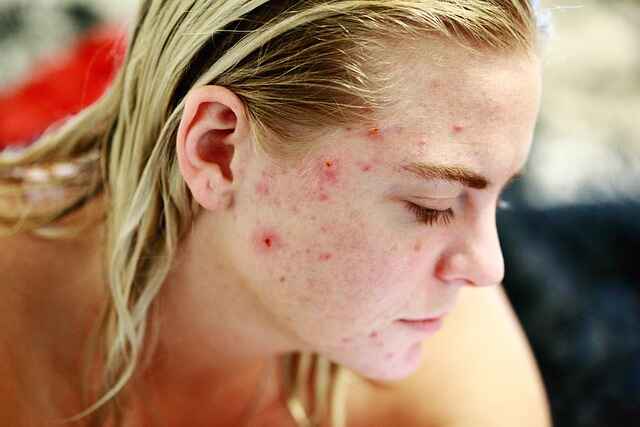
3. Dyshidrotic eczema
Adults under the age of 40 are often affected by Dyshidrotic eczema, also known as pompholyx eczema. It mainly affects the hands and feet, and typical symptoms include severe itching and the development of tiny blisters.
On your hands and feet, it results in the formation of tiny blisters. Men are less likely to have it than women. People are also more likely to get dyshidrotic eczema if they work with specific chemicals or keep their hands submerged in water all day.
4. Discoid eczema
Discoid eczema, also known as nummular eczema, is distinguished by disc-shaped skin areas that are itchy, red, cracked, and swollen. These areas will seem red on those with fair skin.
Darker skin tones may instead generate brown or pale spots. Men are more likely to get discoid eczema, and it tends to get worse during the chilly winter months. The reasons for discoid eczema are not entirely understood, just like those of other forms of eczema. Discoid eczema can form anywhere on the body, but the arms, legs, and torso are where it usually appears.
Also Read: Understanding Diabetes: What is Diabetes? Types, Causes, Symptoms, Management
5. Neurodermatitis
Neurodermatitis is a skin condition that causes persistent itching or scaling.Atopic dermatitis is similar to neurodermatitis. It causes your skin to develop thick, scaly patches. Chronic itching is frequently the first symptom, which usually appears when a patient is going through a difficult or stressful time.
Neurodermatitis is a type of eczema that only affects one or two areas of the skin at a time, as opposed to other types that affect various body parts.
Neurodermatitis patients may have symptoms on their genitalia, shoulders, neck, hands, wrists, or feet. Neurodermatitis in children is uncommon, yet it can occasionally manifest in young atopic dermatitis patients.
6. Stasis dermatitis
Stasis dermatitis, also known as gravity dermatitis, varicose eczema, or venous eczema, is common in older adults.
When fluid seeps into the skin from weak veins, stasis dermatitis develops. Patients who have inadequate leg blood flow or circulation develop stasis dermatitis. Sometimes veins cannot effectively pump blood out of the legs and back toward the heart because of old age or another medical problem.
Stasis dermatitis is more common in women than in males and is directly related to impaired circulation. People who have issues with blood flow in their lower legs experience it. Blood can pool in your legs if the valves which must push blood up through them and toward your heart aren’t working properly.
7. Seborrheic Dermatitis
A typical kind of eczema known as seborrheic dermatitis affects parts of the skin that produce oil, such as the scalp, nose, and upper back
Infants and people between the ages of 30 and 60 are most typically affected by seborrheic dermatitis symptoms. This kind of eczema can cause “cradle cap,” a greasy, scaly patch on the head, in infants. In adults, the condition comes and goes, frequently resurfacing when people are stressed or exposed to cold weather. In infants, the condition usually resolves on its own and does not reoccur.
Dermatologists believe seborrheic dermatitis is caused by an immune system hyper reaction to a yeast overgrowth that occurs naturally on human skin. Seborrheic dermatitis is more common in people who have certain chronic illnesses.
8. Asteatotic eczema
Asteatotic eczema, also known as xerotic eczema and craquelé eczema, often only affects adults over the age of 60. This can be a result of aging skin becoming drier.
Although it can form anywhere on the body, asteatotic eczema commonly affects the lower legs.
Dry skin is a precursor to asteatotic eczema, which most frequently results from environmental conditions. Dry, itchy skin that eventually becomes scaly patches surrounded by narrow, red cracks is the hallmark of this type of eczema.
What causes Eczema?
Eczema’s exact cause is unknown, however, many medical experts concur that a combination of hereditary and environmental factors could be to blame.
If one or both parents have eczema or another atopic disorder, their children are more likely to do as well. If one or both parents have an atopic disorder, the risk can be raised.
Has your child developed a rash on his or her arms, legs, hands, or face? Eczema-related itching can be very bad and frequently keeps people awake at night. Children who scratch their skin risk getting an infection. Babies with eczema might brush against bedding or other objects to get relief from the itching.
Risk Factors
According to several studies, atopic dermatitis affects boys more frequently than girls throughout infancy, with the pattern changing around adolescence.
This skin problem is more likely to affect children whose parents have:
- Atopic dermatitis
- Asthma
- Hash fever

Atopic dermatitis affects people more frequently if they:
- Eat a lot of sugar and polyunsaturated fat in your diet.
- resides in a big city
- Stay in regions with hardly any sun and humidity
- Smoke, or are around smokers
There may be several additional risk factors. These potential risk factors specifically consist of:
- Living in an urban area, or a cold climate
- Being born by a mother who is older than her age
- being a member of a higher socioeconomic class or having educated parents
- being born by a c-section
- Addiction of smoking
- Early childhood exposure to harsh water
- Overweight at the time of birth
Symptoms
Eczema symptoms include:
- a red rash or red patches of skin, particularly inside the elbow and knee folds
- Itching
- Skin that is dry also prone to bleeding and cracking
Although eczema can appear anywhere, it typically affects the scalp, cheeks, inner elbows, backs of the knees, and arms. It is not communicable and occasionally gets milder as you mature.
Many people find it difficult to fall asleep since their symptoms get worse at night. Eczema scratching increases skin inflammation and irritation. This may result in infections that call for antibiotic treatment.
Diagnosis & Treatment
The treatment that is best for you will be determined by the type and severity of your eczema. A dermatologist, allergist, or primary care physician can assist you in determining the best eczema treatment for you.
Dermatologists with specialized training in allergies can treat skin diseases like eczema, which is frequently brought on by an allergic reaction. The kinds of soap, detergent, and skin care products you use, as well as any other exposures that might be exacerbating your eczema, will probably be discussed with you.
Treatment includes
- Medication
- Therapies
- injection of dupilumab
Home Remedy
People with eczema can take a number of steps to maintain skin health and reduce symptoms at home:
- practicing deep breathing techniques
- exercising yoga
- listening to calming music while meditating
- bathing in lukewarm water
- applying moisturizer daily when donning cotton and soft fibers
- Whenever possible, minimize sudden temperature fluctuations and activities that make you sweat
- using a light soap or non-soap cleanser when washing; letting the skin air dry or gently pat it dry with a towel after bathing or taking a shower
- Wherever possible, avoid activities that make you sweat and sudden temperature changes.
- Cutting fingernails short to avoid skin-piercing scratches
Can Eczema be Prevented?
Eczema cannot be cured, but with the correct therapies, the disease’s symptoms can be effectively managed. A balance of medicines and lifestyle changes may be used as treatment.
If you’re having difficulties controlling your eczema or if your symptoms have gotten worse, consult a doctor. They can assist you in identifying a course of treatment that is effective for you and lessens flare-ups.





